Abstract
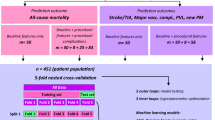
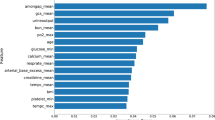
There is high risk of mortality between stage I and stage II palliation of single ventricle heart disease. This study aimed to leverage advanced machine learning algorithms to optimize risk-prediction models and identify features most predictive of interstage mortality. This study utilized retrospective data from the National Pediatric Cardiology Quality Improvement Collaborative and included all patients who underwent stage I palliation and survived to hospital discharge (2008–2019). Multiple machine learning models were evaluated, including logistic regression, random forest, gradient boosting trees, extreme gradient boost trees, and light gradient boosting machines. A total of 3267 patients were included with 208 (6.4%) interstage deaths. Machine learning models were trained on 180 clinical features. Digoxin use at discharge was the most influential factor resulting in a lower risk of interstage mortality (p < 0.0001). Stage I surgery with Blalock-Taussig-Thomas shunt portended higher risk than Sano conduit (7.8% vs 4.4%, p = 0.0002). Non-modifiable risk factors identified with increased risk of interstage mortality included female sex, lower gestational age, and lower birth weight. Post-operative risk factors included the requirement of unplanned catheterization and more severe atrioventricular valve insufficiency at discharge. Light gradient boosting machines demonstrated the best performance with an area under the receiver operative characteristic curve of 0.642. Advanced machine learning algorithms highlight a number of modifiable and non-modifiable risk factors for interstage mortality following stage I palliation. However, model performance remains modest, suggesting the presence of unmeasured confounders that contribute to interstage risk.

Similar content being viewed by others
Abbreviations
- AUROC:
-
Area under the receiver operating characteristic
- BTTs:
-
Blalock-Taussig-Thomas shunt
- CART:
-
Classification and regression tree analysis
- DKS:
-
Damus Kaye Stansel
- ECMO:
-
Extracorporeal membrane oxygenation
- GBT:
-
Gradient boosting trees
- HLHS:
-
Hypoplastic left heart syndrome
- LightGBM:
-
Light gradient boosting model
- ML:
-
Machine learning
- NPC-QIC:
-
National Pediatric Cardiology Quality Improvement Collaborative
- NPV:
-
Negative predictive value
- PPV:
-
Positive predictive value
- REDcap:
-
Research Electronic Data Capture
- RF:
-
Random forest
- SHAP:
-
Shapley additive explanations
- XGBoost:
-
Extreme gradient boosting model
References
Ohye RG, Schranz D, D’Udekem Y (2016) Current therapy for hypoplastic left heart syndrome and related single ventricle lesions. Circulation 134:1265–1279
Kaplinski M, Ittenbach RF, Hunt ML, Stephan D, Natarajan SS, Ravishankar C, Giglia TM, Rychik J, Rome JJ, Mahle M, Kennedy AT, Steven JM, Fuller SM, Nicolson SC, Spray TL, Gaynor JW, Mascio CE (2020) Decreasing interstage mortality after the norwood procedure: a 30-year experience. J Am Heart Assoc 9:e016889
Ghanayem NS, Allen KR, Tabbutt S, Atz AM, Clabby ML, Cooper DS, Eghtesady P, Frommelt PC, Gruber PJ, Hill KD, Kaltman JR, Laussen PC, Lewis AB, Lurito KJ, Minich LL, Ohye RG, Schonbeck JV, Schwartz SM, Singh RK, Goldberg CS, Pediatric Heart Network I (2012) Interstage mortality after the Norwood procedure: Results of the multicenter single ventricle reconstruction trial. J Thorac Cardiovasc Surg 144:896–906
Ohye RG, Sleeper LA, Mahony L, Newburger JW, Pearson GD, Lu M, Goldberg CS, Tabbutt S, Frommelt PC, Ghanayem NS, Laussen PC, Rhodes JF, Lewis AB, Mital S, Ravishankar C, Williams IA, Dunbar-Masterson C, Atz AM, Colan S, Minich LL, Pizarro C, Kanter KR, Jaggers J, Jacobs JP, Krawczeski CD, Pike N, McCrindle BW, Virzi L, Gaynor JW, Pediatric Heart Network I (2010) Comparison of shunt types in the Norwood procedure for single-ventricle lesions. N Engl J Med 362:1980–1992
Ghanayem NS, Hoffman GM, Mussatto KA, Cava JR, Frommelt PC, Rudd NA, Steltzer MM, Bevandic SM, Frisbee SS, Jaquiss RD, Litwin SB, Tweddell JS (2003) Home surveillance program prevents interstage mortality after the Norwood procedure. J Thorac Cardiovasc Surg 126:1367–1377
Furck AK, Uebing A, Hansen JH, Scheewe J, Jung O, Fischer G, Rickers C, Holland-Letz T, Kramer HH (2010) Outcome of the Norwood operation in patients with hypoplastic left heart syndrome: a 12-year single-center survey. J Thorac Cardiovasc Surg 139:359–365
Schidlow DN, Anderson JB, Klitzner TS, Beekman RH 3rd, Jenkins KJ, Kugler JD, Martin GR, Neish SR, Rosenthal GL, Lannon C, Collaborative JNPCQI (2011) Variation in interstage outpatient care after the Norwood procedure: a report from the joint council on congenital heart disease national quality improvement collaborative. Congenit Heart Dis 6:98–107
Anderson JB, Beekman RH 3rd, Kugler JD, Rosenthal GL, Jenkins KJ, Klitzner TS, Martin GR, Neish SR, Brown DW, Mangeot C, King E, Peterson LE, Provost L, Lannon C, Improvement NPCQ, C, (2015) improvement in interstage survival in a national pediatric cardiology learning network. Circ Cardiovasc Qual Outcomes 8:428–436
Oster ME, Kelleman M, McCracken C, Ohye RG, Mahle WT (2016) Association of digoxin with interstage mortality: results from the pediatric heart network single ventricle reconstruction trial public use dataset. J Am Heart Assoc 5(1):e002566
Kugler JD, Beekman Iii RH, Rosenthal GL, Jenkins KJ, Klitzner TS, Martin GR, Neish SR, Lannon C (2009) Development of a pediatric cardiology quality improvement collaborative: from inception to implementation. From the joint council on congenital heart disease quality improvement task force. Congenit Heart Dis 4:318–328
Alsoufi B, McCracken C, Kochilas LK, Clabby M, Kanter K (2018) Factors associated with interstage mortality following neonatal single ventricle palliation. World J Pediatr Congenit Heart Surg 9:616–623
Cross RR, Harahsheh AS, McCarter R, Martin GR, National Pediatric Cardiology Quality Improvement C (2014) Identified mortality risk factors associated with presentation, initial hospitalisation, and interstage period for the Norwood operation in a multi-centre registry: a report from the national pediatric cardiology-quality improvement collaborative. Cardiol Young 24:253–262
Cua CL, Thiagarajan RR, Taeed R, Hoffman TM, Lai L, Hayes J, Laussen PC, Feltes TF (2005) Improved interstage mortality with the modified Norwood procedure: a meta-analysis. Ann Thorac Surg 80:44–49
Fernandez RP, Joy BF, Allen R, Stewart J, Miller-Tate H, Miao Y, Nicholson L, Cua CL (2017) Interstage survival for patients with hypoplastic left heart syndrome after ECMO. Pediatr Cardiol 38:50–55
Ghanayem NS, Allen KR, Tabbutt S, Atz AM, Clabby ML, Cooper DS, Eghtesady P, Frommelt PC, Gruber PJ, Hill KD, Kaltman JR, Laussen PC, Lewis AB, Lurito KJ, Minich LL, Ohye RG, Schonbeck JV, Schwartz SM, Singh RK, Goldberg CS (2012) Interstage mortality after the norwood procedure: results of the multicenter single ventricle reconstruction trial. J Thorac Cardiovasc Surg 144:896–906
Hebson CL, Oster ME, Kirshbom PM, Clabby ML, Wulkan ML, Simsic JM (2012) Association of feeding modality with interstage mortality after single-ventricle palliation. J Thorac Cardiovasc Surg 144:173–177
Brown DW, Mangeot C, Anderson JB, Peterson LE, King EC, Lihn SL, Neish SR, Fleishman C, Phelps C, Hanke S, Beekman RH, Lannon CM, National Pediatric Cardiology Quality Improvement C (2016) Digoxin use is associated with reduced interstage mortality in patients with no history of arrhythmia after stage I palliation for single ventricle heart disease. J Am Heart Assoc 5(1):e002376
Song J, Kang IS, Huh J, Lee OJ, Kim G, Jun TG, Yang JH (2013) Interstage mortality for functional single ventricle with heterotaxy syndrome: a retrospective study of the clinical experience of a single tertiary center. J Cardiothorac Surg 8:93
Taylor LC, Burke B, Donohue JE, Yu S, Hirsch-Romano JC, Ohye RG, Goldberg CS (2016) Risk Factors for interstage mortality following the norwood procedure: impact of sociodemographic factors. Pediatr Cardiol 37:68–75
Ahmed H, Anderson JB, Bates KE, Fleishman CE, Natarajan S, Ghanayem NS, Sleeper LA, Lannon CM, Brown DW, National Pediatric Cardiology Quality Improvement C (2020) Development of a validated risk score for interstage death or transplant after stage I palliation for single-ventricle heart disease. J Thorac Cardiovasc Surg 160:1021–1030
Zhao J, Feng Q, Wu P, Lupu RA, Wilke RA, Wells QS, Denny JC, Wei WQ (2019) Learning from longitudinal data in electronic health record and genetic data to improve cardiovascular event prediction. Sci Rep 9:717
Yan C, Gao C, Zhang Z, Chen W, Malin BA, Ely EW, Patel MB, Chen Y (2021) Predicting brain function status changes in critically ill patients via Machine learning. J Am Med Inform Assoc 28:2412–2422
Hyland SL, Faltys M, Huser M, Lyu X, Gumbsch T, Esteban C, Bock C, Horn M, Moor M, Rieck B, Zimmermann M, Bodenham D, Borgwardt K, Ratsch G, Merz TM (2020) Early prediction of circulatory failure in the intensive care unit using machine learning. Nat Med 26:364–373
Wright MN (2021) ranger: A Fast Implementation of Random Forests.
Chen T, Guestrin C (2016) XGBoost: A Scalable Tree Boosting System. Proceedings of the 22nd ACM SIGKDD International Conference on Knowledge Discovery and Data Mining. Association for Computing Machinery, San Francisco pp 785–794
Natekin A, Knoll A (2013) Gradient boosting machines, a tutorial. Front Neurorobot 7:21
Kopitar L, Kocbek P, Cilar L, Sheikh A, Stiglic G (2020) Early detection of type 2 diabetes mellitus using machine learning-based prediction models. Sci Rep 10:11981
Osawa I, Goto T, Yamamoto Y, Tsugawa Y (2020) Machine-learning-based prediction models for high-need high-cost patients using nationwide clinical and claims data. npj Digital Medicine 3:148
Lundberg SM, Lee S-I (2017) A unified approach to interpreting model predictions. Proceedings of the 31st International Conference on Neural Information Processing Systems. Curran Associates Inc., Long Beach pp 4768–4777
Lundberg SM, Erion G, Chen H, DeGrave A, Prutkin JM, Nair B, Katz R, Himmelfarb J, Bansal N, Lee S-I (2020) From local explanations to global understanding with explainable AI for trees. Nature Machine Intelligence 2:56–67
Newburger JW, Sleeper LA, Frommelt PC, Pearson GD, Mahle WT, Chen S, Dunbar-Masterson C, Mital S, Williams IA, Ghanayem NS, Goldberg CS, Jacobs JP, Krawczeski CD, Lewis AB, Pasquali SK, Pizarro C, Gruber PJ, Atz AM, Khaikin S, Gaynor JW, Ohye RG, Pediatric Heart Network I (2014) Transplantation-free survival and interventions at 3 years in the single ventricle reconstruction trial. Circulation 129:2013–2020
Klausner RE, Parra D, Kohl K, Brown T, Hill GD, Minich L, Godown J (2021) Impact of digoxin use on interstage outcomes of single ventricle heart disease (From a NPC-QIC Registry Analysis). Am J Cardiol 154:99–105
Klausner RE, Godown J (2020) Digoxin utilization following the Norwood procedure in patients with hypoplastic left heart syndrome: a multicenter database analysis. Prog Pediatr Cardiol 59:101299
Van Hare GF (2019) Perspective. Digoxin for interstage single ventricle patients: what could possibly go wrong? Congenit Heart Dis 14:321–323
Varghese J, Hammel JM, Ibrahimiye AN, Siecke R, Bisselou Moukagna KS, Kutty S (2019) Outcomes related to immediate extubation after stage 1 Norwood palliation for hypoplastic left heart syndrome. J Thorac Cardiovasc Surg 157:1591–1598
Arnaout R, Curran L, Zhao Y, Levine JC, Chinn E, Moon-Grady AJ (2021) An ensemble of neural networks provides expert-level prenatal detection of complex congenital heart disease. Nat Med 27:882–891
Helman SM, Herrup EA, Christopher AB, Al-Zaiti SS (2021) The role of machine learning applications in diagnosing and assessing critical and non-critical CHD: a scoping review. Cardiol Young 31:1770–1780
Acknowledgements
None
Funding
Dr. Sunthankar received funding from NIH T32 5T32HL105334-10 and Project Heart. Dr. Jayaram is supported by a Career Development Award (K23HL153895) from the NHLBI.
Author information
Authors and Affiliations
Contributions
All authors have contributed in a significant and meaningful way deserving of authorship. SDS, JZ, WQW, and JG designed the study. SDS, GDH, DAP, KK, NMJ, JG all have expertise in single ventricle congenital heart disease. GDH, AM, NMJ are intimately involved with the NPC-QIC registry and served as resources for data acquisition. JZ and WQW have expertise in machine learning models and completed the statistical analysis. SDS, JZ, and JG were involved in clinical interpretation of machine learning models and manuscript preparation. All authors have read and approved the submitted version and no authors have financial or other relationships that might lead to a conflict of interest.
Corresponding author
Ethics declarations
Competing interests
The authors declare no competing interests.
Additional information
Publisher's Note
Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Supplementary Information
Below is the link to the electronic supplementary material.
Rights and permissions
Springer Nature or its licensor (e.g. a society or other partner) holds exclusive rights to this article under a publishing agreement with the author(s) or other rightsholder(s); author self-archiving of the accepted manuscript version of this article is solely governed by the terms of such publishing agreement and applicable law.
About this article
Cite this article
Sunthankar, S.D., Zhao, J., Wei, WQ. et al. Machine Learning to Predict Interstage Mortality Following Single Ventricle Palliation: A NPC-QIC Database Analysis. Pediatr Cardiol 44, 1242–1250 (2023). https://doi.org/10.1007/s00246-023-03130-z
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s00246-023-03130-z